|
Diabetes
Am I at risk for type II diabetes?
I have Diabetes, What should I eat?
I have Diabetes, How Much should I eat?
Keep Your Diabetes Under Control
Introduction
What is Diabetes?
Two Types of Diabetes Mellitus
Symptoms of NIDDM
Diagnosis of Diabetes
Complications of Diabetes
Importance of Tight
Blood Sugar Control
Type II Diabetes - Curable?
Diabetes Protocol
1. Key Nutritional Supplements
A. Chromium
B. VITAMIN C
C. VITAMIN E
D. Digestive enzymes
E. Magnesium
2. Auxiliary Supporting
nutrients
3. Diabetic Low Glycemic
Index Diet
Anti-Aging Food Pyramid
for Diabetes
Diet Tips for Diabetes
Mellitus
4 . Exercise
5. Prescription Medications
Summary
Introduction
 Of the 15 million Americans who have
Type II diabetes, more than a third don't know it. Another 21 million Americans have a greater than 50-50
chance of developing the disease because they have impaired blood-sugar
metabolism. This year alone more
than 187,000 people will die of Type II diabetes, also called
non-insulin-dependent diabetes mellitus (NIDDM), making it the
sixth leading cause of death by disease. Each day, over 2,200
people are diagnosed with this chronic life debilitating,
expansive,
and pro-aging disease. Of the 15 million Americans who have
Type II diabetes, more than a third don't know it. Another 21 million Americans have a greater than 50-50
chance of developing the disease because they have impaired blood-sugar
metabolism. This year alone more
than 187,000 people will die of Type II diabetes, also called
non-insulin-dependent diabetes mellitus (NIDDM), making it the
sixth leading cause of death by disease. Each day, over 2,200
people are diagnosed with this chronic life debilitating,
expansive,
and pro-aging disease.
What is Diabetes?
Glucose is a simple sugar found in food. It is an essential nutrient
that provides energy for the proper functioning of the body cells.
After meals, food is digested in the stomach and the intestine
to glucose and other nutrients. The glucose in digested food is
absorbed by the intestinal cells into the bloodstream, and
is carried by blood to all the cells in the body. However, glucose
cannot enter the cells alone. It needs assistance from insulin
to penetrate the cell walls. Insulin therefore acts as
a regulator of glucose metabolism in the body.
Insulin is called the "hunger hormone". As the blood sugar
level increases following a carbohydrate rich meal, the corresponding
insulin level rises with the eventual lowering of the blood sugar
level and glucose is transported from the blood into the cell
for energy. When the blood glucose levels are lowered, the insulin
release from the pancreas is turned off. When the blood sugar
level drops below a certain level, hunger is felt. This often
occurs a few hours after the meal. In normal individuals, such
a regulatory system helps to keep blood glucose levels in a tightly
controlled range. Cravings for sweets frequently form part of
this cycle, which can lead to snacking, often for more carbohydrates.
If the cravings are not fulfilled, sensations such as hunger,
dizziness, moodiness, and a state of "collapse" can result.
This system of auto regulation and homeostasis is the function
of the pancreas and it works around the clock. Dysfunction of
this auto regulation system - either inability of the pancreas
to secret any or insufficient insulin, or pancreas overload from
too much sugar ingested over a long period of time, or over compensatory
mechanism, or a combination of these, results in the lack of
insulin, and hence high blood sugar. This is the hallmark of diabetes
mellitus (commonly called diabetes)
Two Types of Diabetes Mellitus
-
Type
I diabetes mellitus is also called insulin dependent diabetes
mellitus (IDDM), or juvenile onset diabetes mellitus.
It is an autoimmune disease in which the pancreas produces
no insulin at all, and the patient relies on insulin medication
for survival. Type I diabetes tends to occur in young, lean
individuals, usually before 30 years of age. Approximately
10% of the patients with diabetes mellitus have IDDM. There
is no cure for this type.
-
Type
II diabetes mellitus is also referred to as non-insulin dependent
diabetes mellitus (NIDDM), or adult onset diabetes mellitus
(AODM). It is a metabolic disorder resulting from
the body's inability to make enough, or properly use, insulin.
90% of all Diabetes Mellitus are of Type II. Type II diabetes
mellitus occurs mostly in individuals over 40 years old. The
incidence of type II diabetes increases with age. Unlike type I diabetes mellitus, 80%
of type II diabetic patients are obese.
Type II diabetes mellitus also has a strong genetic
tendency.
It is nearing epidemic proportions, due to an increased number
of elderly people, a greater prevalence of obesity and
a sedentary lifestyle. In type II diabetes, patients can still
produce insulin, but do so inadequately. The pancreas in these
patients not only produces an insufficient amount of insulin,
but also releases insulin late in response to increased glucose
levels. Some type II diabetics have body cells that are resistant
to the action of insulin (Insulin Resistance). Finally, the
liver in these patients continues to produce glucose despite
elevated glucose levels.
Type II diabetes once hardly ever struck before middle
age, and the older you are the more at risk you are. Now it
is striking younger people.
Symptoms of NIDDM
 The early symptoms of untreated diabetes mellitus are related to
elevated blood sugar levels, and
excretion of it to the urine. High amounts of glucose
in the urine can cause increased urine output and lead to dehydration. Dehydration causes increased thirst and water
consumption. Some untreated diabetic patients also complain of
fatigue, nausea, and vomiting. Patients with diabetes are prone
to developing infections of the bladder, skin, and vaginal areas.
Fluctuations in blood glucose levels can lead to blurred vision.
Extremely elevated glucose levels can lead to lethargy and coma (diabetic coma). The early symptoms of untreated diabetes mellitus are related to
elevated blood sugar levels, and
excretion of it to the urine. High amounts of glucose
in the urine can cause increased urine output and lead to dehydration. Dehydration causes increased thirst and water
consumption. Some untreated diabetic patients also complain of
fatigue, nausea, and vomiting. Patients with diabetes are prone
to developing infections of the bladder, skin, and vaginal areas.
Fluctuations in blood glucose levels can lead to blurred vision.
Extremely elevated glucose levels can lead to lethargy and coma (diabetic coma).
The most unrecognized symptom of NIDDM is weight gain.
High insulin levels prohibit the release of serotonin, a neurotransmitter
in the brain that informs the body to slow down eating. Without
serotonin, there is a tendency to overeat, which then leads to
a spiral of excessive sugar intake. A viscous cycle of hyper-insulinemia
resulting in insulin resistance is set up. This in turn creates
a "carbohydrate addict" whose craving for
a higher sugar intake continues to increase. The same dietary
factors that cause NIDDM lead to obesity. Eating refined carbohydrates
such as sugar, or carbohydrates that easily converts into sugar
such as yam, potato, or rice, creates more glucose than the body
can handle. Excess glucose then gets stored as fat. As diabetes
sets in, so does lethargy and inactivity, contributing further
to the vicious
cycle of weight gain and worsening of diabetes.
Diagnosis of Diabetes
The fasting plasma glucose test is the standard and preferred
way to diagnose diabetes. Normal fasting plasma glucose levels
are less than 110 milligrams per deciliter (mg/dl). If the overnight
fasting blood glucose is greater
than 126 mg/dl on two different tests on different days,
the diagnosis of diabetes mellitus is made. Random blood glucose
alone is seldom used because it is not reliable.
Fasting
blood sugar can be performed using a simple home blood sugar
(glucose) testing kit. Many doctors also take the hemoglobin A1C
level. This is a test to measure of the overall effectiveness
of blood glucose control over a period of time (two months). Elevated
hemoglobin A1C levels indicate a poor overall control of blood
sugar.
Complications of Diabetes
Type 1 Diabetes:
Insulin is vital to patients with
type I diabetes. Without insulin, patients with type I diabetes
can develop severely elevated blood sugar levels. This leads to
increased urine glucose, which in turn leads to excessive loss
of fluid and electrolytes in the urine. Lack of insulin also causes
the breakdown of fat cells, with the release of ketones into the
blood. Symptoms of diabetic ketoacidosis include nausea,
vomiting, and abdominal pain. Without prompt medical treatment,
patients with diabetic acidosis can rapidly go into shock, coma,
and even death. With proper treatment, the symptoms can be reversed
rapidly, and patients can recover remarkably well.
Type 2 Diabetes:
Short term complications
are normally due imbalance of sugar level in the body as a result
of:
A. Severely high blood sugar levels
due to a lack of insulin. Symptoms are similar to that
of Type 1 Diabetes described above.
B. Abnormally low blood sugar levels due to too much
insulin or other glucose-lowering medications. Low
blood sugar can lead to nervous system symptoms such as dizziness,
confusion, weakness, and tremors. Untreated, severely low blood
sugar levels can lead to coma and irreversible brain death.
Long-term complications
are related to blood vessel diseases. Diabetes causes diseases
of the small vessels, which can damage the eyes, kidneys, nerves,
and heart. Four major areas are involved:
A. EYE. Each year about 24,000 people lose their
sight because of diabetes. Diabetes is the main cause of blindness
in adult. Eye complications of diabetes (diabetic retinopathy)
occur in patients who have had diabetes for at least 5 years.
Disease in these blood vessels also causes the formation of small
aneurysms (micro aneurysms), and new but brittle blood vessels
(neovascularization). Spontaneous bleeding from the new and brittle
blood vessels can lead to retinal scarring and retinal detachment,
thus impairing vision. Approximately 50% of patients with diabetes
will develop some degree of diabetic
retinopathy after 10 years of diabetes, and 80% of diabetics
have retinopathy after 15 years of the disease.
B. Kidney damage from diabetes is called
diabetic nephropathy. Kidney disease usually occurs approximately
10 years after the onset of diabetes. Each year, about 28,000
people initiated treatment for end stage renal disease (kidney
failure) because of diabetes. The progression of nephropathy in
patients can be significantly slowed by controlling high blood
pressure, and by aggressively treating high blood sugar levels.
C. Nerve damage in diabetes (diabetic neuropathy)
is also caused by small blood vessel disease. Symptoms of diabetic
nerve damage include numbness, burning, and aching of the feet
and lower extremities. Seemingly minor skin injuries should be
attended to promptly to avoid serious infections. Diabetic nerve
damage can affect the nerves, which are important for penile erection,
causing impotence. Diabetic neuropathy can also affect nerves
to the intestines, causing nausea, weight loss, and diarrhea.
About 60-70% of people with diabetes have mild to sever form of
diabetic nerve damage. The risk of a leg amputation
is 15-40 times greater for a person with diabetes. Each year,
more than 56,000 amputations are performed among people with diabetes.
D. Heart Disease and Strokes. Patients with diabetes are
2-4 times more likely to have
heart disease, which is present in 75 percent of diabetes-related
death (more than 75,000 deaths due to heart disease annually).
Diabetic patients are also 2 to 4 times more like to suffer a
stroke. Diabetes also accelerates hardening of the arteries (atherosclerosis)
of the larger blood vessels, leading to coronary heart disease
(angina or heart attack), strokes, and pain in the lower extremities
because of lack of blood supply.
Diabetic men were more than twice as likely to die of all causes
compared with men without diabetes. As blood glucose increased,
the risk of dying climbed higher regardless of age, weight, blood
pressure, cholesterol and smoking status.
Researchers estimated that a reduction
in blood glucose by just 0.1 per cent could reduce mortality rates
by about five per cent in Western country
Importance of Tight Blood
Sugar Control
An aggressive and intensive control of elevated levels of blood
sugar in patients with diabetes is absolutely essential. Studies
have shown that in intensively treated patients, diabetic eye
disease decreased by 76%, kidney disease decreased by 54%, and
nerve disease decreased by 60%.
Aggressive control with intensive therapy means achieving fasting
glucose levels between 70-120 mg/dl; glucose levels of less than
180 mg/dl after meals; and a near normal hemoglobin A1C levels.
Not only will you feel better, stay healthy, and have more energy.
You will also live longer.
Type II Diabetes - Curable?
Diabetes is a disease that has
become prevalent only in the past 100 years. Before then,
when everyone ate whole foods and sugar intake is moderate, diabetes
was hardly a problem.
It's a simple of matter of supply and demand. If the ingestion
of grain products and refined sugar exceed the demand, the body
is put on high gear to rid itself of the excess sugar. Diabetes
is resulted when this process carries on for an extended period
of time and ultimately fails. No
other disease state can be cured
as easily as NIIDM.
All you have to do is to reduce the supply
of sugar to the body to a moderate level without sacrificing
energy production. The secret lies not in avoiding carbohydrates as the most common
source of sugar. The key is knowing
what kind of carbohydrate to take and which kind to
avoid
Diabetes Protocol
The major goal in treating diabetes
mellitus is controlling elevated blood sugars (glucose) without
causing abnormally low levels of blood sugar. Type I diabetes
mellitus is treated with insulin, exercise, and a diabetic diet.
Type II diabetes mellitus is treated with
concurrent employment of nutritional
supplements, a low glycemic index diet to control blood
sugar level, and exercise. If these measures
fail to contain the elevated blood sugars, oral medications and
insulin needs to be considered.
1. Key Nutritional Supplements
A VARIETY OF NUTRIENTS
AND HERBS can help offset
the toll diabetes takes on your body. Supplements cannot,
however, reverse the disease by themselves. Incorporating these
minerals and vitamins can help to normalize blood sugar. If you
already have diabetes or suspect you might have it, consult
a health care practitioner before taking any supplements.
A. Chromium:.
Chromium is an
essential trace mineral nutrient. Like iron, zinc, selenium, copper,
and several other essential trace minerals, chromium plays a critical
role in maintaining normal health and well-being.
Chromium helps insulin to work efficiently. Many well controlled
clinical studies through the years and the majority shows blood
glucose improvements in the patients tested.
Important studies include one from the Human Nutrition Research
Center of the United States Department of Agriculture conducted
in 1996. Researchers in the study randomized 180 adult-onset diabetics
into 3 groups of 60 each: one group received placebo twice per
day, the second received 100 mcg twice daily of chromium as chromium
picolinate and the third received 500 mcg of chromium as chromium
picolinate twice daily. Their blood work was examined at baseline,
at 2 months and at 4 months. The patients were told to remain
on their anti-diabetic medications and continue with their diets
and activity levels as before. The results were impressive: blood
glucose, insulin levels, cholesterol and Hemoglobin A1C all decreased,
with the higher dose generally (but not always) more effective
than the 200 mcg.
Dietary Intake of Chromium
Few foods are rich sources of chromium in the Western diet, the
best being organ meats, mushrooms, wheat germ, broccoli and processed
meats. Data from U. S. Government sources show that the great
majority of Americans get less chromium in their daily diets than
the amount recommended by nutrition experts.
The RDA Committee recommends 50-200 mcg of chromium/day; the vast
majority of Americans get less than 50 mcg/day. It is estimated that as high as 80% of all Americans is deficient
in this mineral and may not know it.
Unfortunately, it is not possible to get enough chromium by
food alone without excessive calories and obesity. To obtain
200 mcg by food alone, one has to take in over 8,000 calories
a day. A large part of the problem
has to do with processed food and the increase consumption of
sugar. The modern American consumes an average of 120
pounds of sugar per year from all sources. These ingested sugars
(such as table sugar and products made with it) bring insulin
and chromium into the blood and cause chromium to be excreted
in the urine after it's through working with the insulin on the
increase in blood sugar.
Inadequate chromium intake from processed food, increased chromium
losses due to increased sugar consumption, decreasing chromium
tissue levels as we age are the main reasons why the majority
of Americans and diabetics are deficiency in chromium. StudImprovement
in blood sugar in significant numbers of diabetics and pre-diabetics
with modest chromium supplementation. It should, however,
takes place alongside the two other proven ways of normalizing
sugar: low-fat, high complex-carbohydrate of low glycemic index
type diets for weight loss/weight maintenance and regular exercise.
Assessment of Chromium Status
Deciding whether or not someone is chromium deficient cannot be
done easily. Routine blood test is generally not accurate.
The only generally accepted method
for assessment of chromium status is to supplement an individual
who has abnormalities of either blood sugar, cholesterol, triglycerides
or all three with the trace clement. If the laboratory values
improve, then chromium insufficiency is presumed.
Safety of Chromium
Chromium comes in various forms. The dietary form is called chromium tri-valent. This
is non-toxic and necessary for essential body function. Chromium
in its hexa-valent form is used in industries and that is highly
toxic.
It is extremely difficult to poison laboratory animals with
oral dietary tri-valent form of chromium. For example, cats
fed 1,000 mg of trivalent chromium per day showed no signs of
toxicity. The equivalent daily dose for a 150 lb person would
be approximately 35,000 mg per day or 3.5 million mcg per day.
In terms of the number of 200 mcg tablets, this would be 175,000
tablets per day for a human.
"Trivalent chromium has such a low order of toxicity that deleterious
effects from excessive intake of this form of chromium do not
occur readily. Trivalent chromium becomes toxic only at extremely
high amounts - chromium then acts as a gastric irritant rather
than as a toxic element interfering with essential metabolism
or biochemistry." Modern Nutrition In Health and Disease, Eighth
Ed., 1994. Shils, Olson and Shike, eds.
The safety issue had been question by a study published in December
1995, which attempted to link chromosomal damage in the test tube
to oral supplementation of chromium picolinate. Researchers in
this study added unnaturally high amounts of chromium picolinate
to cultured Chinese hamster ovarian cancer. Some of these cells
showed chromosomal damage. This was not particularly surprising,
since this concentration applied was 3,000 times the blood level
of people who are ingesting chromium picolinate as supplements.
It is interesting to note that another form of chromium, chromium
polynicotinate, did not have this toxic effect.
It is important to note that very few essential minerals tested
in this way would be found to be without toxicity. For example,
merely doubling the blood concentration of the mineral calcium
is fatal to humans.
A further study was conducted by Dr. Richard Anderson, the lead
scientist for trace minerals at the U.S. Department of Agriculture's
Human Nutrition Research Center, Beltsville, Md., His research
team fed rats a stock diet . Added to the diet was 0, 5,
25, 50 or 100 micrograms (mcg) of chromium per gram of feed for
a period of six months. The supplements were added to the feed
in the form of chromium chloride or chromium picolinate. The highest
supplemented level measured approximately 1500 mcg/day per kilogram
of body weight. Translated to human equivalent would mean that
a 150 lb (70 kg) individual would have to consume 1.05 million
micrograms, or more than 5,000 tablets containing 200 mcg
of chromium each daily for six months to equal the rat intake.
This study found no harmful effects in animals supplemented
with two widely used forms of dietary chromium: chromium chloride
and chromium picolinate.
Forms of Chromium
There are various forms of dietary chromium. These vary
in bioavailability (absorption and retention) and biological activity
(ability to potentate and harmonize insulin). Inorganic
chromium such as chromium chloride is unfortunately poorly
absorbed (0.5-2%) and has little effect on insulin because it
must first be converted into a biologically active form, which
the body has a limited ability to do.
The two most popular forms of organic chromium are niacin-bound
chromium (also called chromium polynicotinate) and chromium picolinate.
Although picolinate and polynicotinate sound alike, there are
significant differences between the two compounds.
Chromium Polynicotinate is actually a family of niacin-bound chromium
compounds. Niacin-bound chromium strongly potentiates insulin
- chromium's most vital function - while chromium picolinate is
less effective comparatively speaking.
Niacin-bound chromium such as chromium
polynciotinate is also more bioavailable than chromium picolinate.
An Animal study at the University of California found that
chromium polynicotinate is better absorbed and retained up to
311% better than chromium picolinate and 672% better than chromium
chloride. Such high bioavailability means that chromium polynicotinate
can deliver more of the benefits that chromium has to offer.
B. VITAMIN C:
As a strong antioxidant, this vitamin
enhances capillary strength, which improves blood flow. Dietary
sources include leafy greens, broccoli, peppers, oranges, and
grapefruit are the primary source of dietary vitamin C,
followed by commercial supplements.
Vitamin
C administration has beneficial effects on sugar and fat metabolism
in NIIDM. In a randomized double-blind cross-over study, in which
56 diabetic patients participated, it has been established that
a supplementation of a high doses of ascorbic
acid (2 grams a day) markedly improves the blood sugar regulation
in patients with NIDDM. It was recorded that the vitamin
C supplementation in the NIDDM group resulted in a statistically
significant decrease of the fasting blood sugar of 10.1 to 9.1
mmol/liter. In this group the vitamin C supplement also succeeded
in lowering the level of LDL cholesterol and of triglycerides
in the blood. The greater the amount of vitamin C taken, the
greater reduction in LDL cholesterol and plasma free radicals.
The plasma free radicals are also lower compared to the placebo
group. This was reported in the Journal of the American College
of Nutrition (Aug. 1995).
 Vitamin C also reduces the potential of complications
arising from persistent high sugar environment in the body. Specifically,
vitamin C prevents accumulation of sorbitol (a sugar equivalent)
in cells and protect against most complications resulting from
oxidation. A large population based
study found that patients with high blood levels of Vitamin C
had a lower HbA1C. Vitamin C also reduces the potential of complications
arising from persistent high sugar environment in the body. Specifically,
vitamin C prevents accumulation of sorbitol (a sugar equivalent)
in cells and protect against most complications resulting from
oxidation. A large population based
study found that patients with high blood levels of Vitamin C
had a lower HbA1C.
Furthermore, patients with diabetes have low levels of Vitamin
C in the cells, which can results in impaired wound healing. High
dose supplements have been shown to prevent sorbitol accumulation
and glycosilation of proteins in, both of which are important
factors in development of diabetic complications such as cataract.
1 to 2 gram daily of Vitamin C is recommended for diabetic
patients.
C. VITAMIN E:
Vitamin E reduces oxidative stress, thus improving membrane physical
characteristics and related activities in glucose transport.
This antioxidant promotes healing of diabetes-related lesions,
whose cause is undetermined. Researchers have extensively investigated
the possible effects of vitamin E supplementation on the cardiac
autonomic nervous system in patients with type 2 diabetes and
cardiac autonomic neuropathy. It was reported in the American
Journal of Clinical Nutrition that daily vitamin
E supplementation (600 mg) for 4 months improved the ratio
of cardiac sympathetic to parasympathetic tone in patients with
NIIDM. This effect might be mediated by a decline in oxidative
stress. In short, Vitamin E (800 to 1200 I.U.) improves insulin action
and prevents a host of long-term complications of diabetes including
neuropathy.
In another study, 21 NIIDM patients with microangiopathic complications
were divided into 2 groups, in which 11 patients took 900 mg of
vitamin E daily and the other group of 10 diabetic patients took
a placebo daily for 6 months. The vitamin E was provided in tablets
containing 100 mg of dl-alpha-tocopheryl acetate. The mean age
of these subjects was 58 years. This study showed that these diabetic
patients had impaired erythrocyte osmotic fragility, and that
pharmacological doses of vitamin E increased the resistance of
erythrocytes to osmotic hemolysis in patients with microangiopathy.
Vitamin E also appears to play a significant role in the prevention
of diabetes. Studies have shown
that a low vitamin-E concentration
was associated with 3.9 times greater risk of developing diabetes.
D. Digestive enzymes:
Largely because of our modern diets, which are deficient in enzymes,
most of us deplete our body's natural enzyme level as we age.
Tests have shown that a 70-year-old person has only about half
the enzyme level of a 20-year-old. A newborn baby has 100
times the enzymes levels of an elderly person! As we become enzyme-deficient,
we age faster. Lack of enzymes also puts stress on vital organs
like the pancreas, liver and spleen, causing a metabolic deficit.
Unfortunately, cooking any food at temperatures above above 116
degrees Fahrenheit kills all enzymes. All canned or bottled foods
contain no enzymes because they are cooked before being processed.
Raw vegetables and fruits can be an excellent natural source of
enzymes if they are allowed to ripen. Unfortunately, they
contain no enzymes when they are picked "green" (often the case
in supermarkets because they have to be transported over long
distances). Enzymes can only develop when they ripen on the plant.
Irradiating food, or treating it with preservatives can also kill
enzymes.
Enzymes in raw food can actually digest as much as 75 percent
of the food itself without help of enzymes secreted by your body.
Without sufficient enzyme levels, the foods you eat can't be completely
broken down and absorbed. Diabetics
have a greatly weakened state of their pancreas and digestive
tract. Two common efficient
in the diabetic are lipase and amylase.
-
Lipase. The lipase
level in the pancreatic juice of many diabetics was found
to be decreased. Most people associate diabetes with sugar
intolerance, but fat intolerance is the major enzyme culprit.
The inability to digest fat interferes with insulin metabolism
and the transport of glucose into the cell by insulin. Lipase
breaks down neutral fats (triglycerides) into glycerol (an
alcohol) and fatty acids (see quick definition). Lipase
deficiency is therefore associated with diabetes and glucosuria
(sugar in the urine without symptoms of diabetes).
E. Magnesium:
Magnesium
is involved in many areas of glucose metabolism. Its deficiency is common among diabetics. Supplementation
of magnesium may prevent some of the complications of diabetes,
such as retinopathy and heart
disease. The RDA for magnesium is 350 mg day for adult
males and 300 mg for adult female. The
diabetic may need 700 mg. The average diet contains
about 200 mg a day, so the majority of adults are deficient. Magnesium
occurs abundantly in whole foods such as seeds, nuts, whole grains,
and green leafy vegetable, but food processing takes out a large
portion. In addition to magnesium at least 50 mg of vitamin
B6 should be taken, as the level of intracellular vitamin
B6 appears to be linked to the magnesium content of the cell.
Without adequate B6, magnesium's entrance into the cell is impaired.
2. Auxiliary Supporting nutrients
A. ALPHA-LIPOIC ACID: Lipoic
Acid is an antioxidant that is especially effective for the
treatment of diabetic poly neuropathy- the nerve degeneration
that often accompanies diabetes - which causes pain, tingling,
and numbness in the hands and feet. Red and organ meats are the
richest dietary sources, but it is also found in carrots, yams,
beets, and spinach. Take 300-500 mg a day.
B. BITTER MELON: A member of the squash family, this plant
normalizes glucose levels and is used as the sole remedy for diabetes
in some parts of China and India. Clinical trials have shown good
results with NIIDM who were given 2 ounces of the juices. Drink
2 ounces of the juice daily for the first week, and then increase
the dose to 8 ounces.
C. BLUEBERRY: Incorporating this fruit into your diet on
a regular basis helps protect your arteries and nerves from damage
due to diabetes. Eat at least 1/2 cup of fresh berries every day,
or take 25 mg capsules two times a day.
D. Bilberry (European Blueberry): This is a plant from
Europe. Bilberry leaf tea has a long history of folk use in the
treatment of diabetes. This use is supported by research which
has shown that oral intake reduce blood sugar level in normal
and diabetic animals. Bilberry flavonoids (anthocyanosides) have
been shown to increase intracellular vitamin C level, decrease
the leakiness and breakage of small vessels commonly associated
with vascular damage from diabetes. Has an affinity for blood
vessels of the eye and retina, and improves circulation t the
retina. This affinity is consistent with several clinical trails
showing positive results with diabetic retinopathy. The dose widely
used in Europe is standardized to contain 25% anthocyanidine.
Take 50 mg to 100 mg three times a day.
E. VITAMIN A: This antioxidant helps convert beta-carotene
efficiently, which reduces the risk of blindness in diabetics.
Foods rich in vitamin A include green leafy vegetables, sweet
potatoes, fish, watermelon, and cantaloupe. Take 2,500 I.U.
daily.
F. ZINC: Diabetics typically excrete excessive amounts
of zinc
in the urine and therefore require supplementation. Taken daily,
this mineral helps control blood-sugar levels. Take 30 mg a
day.
G. GINKGO BILOBA: Gingko has been
shown to improve cerebral
and peripheral vascular blood flow. This is important for
diabetics who commonly suffer from peripheral vascular insufficiency.
Dosage is standardized to contain 24% gingko flavoglyosides. Take
40 to 80 mg three times a day.
H. GYMNEA SYLVESTRE: This Ayurvedic medicine has been used
in India for centuries to improve blood-sugar levels. It works
to regenerate the insulin-producing beta cells in the pancreas.
Gymnea extract has shown positive clinical results in reduce blood
sugar in both Type I and II diabetics. It is interesting to note
that no blood-sugar-lowering effect is seen in healthy volunteers.
Take 200 mg 1 -2 times a day.
I. Vitamin B12: Vitamin B12
supplementation has been used successfully to treat diabetic neuropathy.
Vitamin
B12 deficiency is characterized by numbness of the feet, pins-and-needles
sensation, or a burning feeling - common symptoms of diabetic
neuropathy. Oral supplementation with 500 to 2,000 mcg per
day is usually sufficient.
J. Vanadium: The amount of vanadium we get in our
diet appears to be 50-60 mcg. In the therapeutic use in diabetes
management, dosage required is often 1000-fold greater. Unfortunately,
vanadium compounds have not been extensively tested in clinical
trails. The use of vanadium for treatment of diabetes should best
be taken under the supervision of a knowledgeable physician.
K. FISH OILS: These oils
help improve insulin efficiency by enhancing blood flow to arteries
and reducing the clumping of red blood cells. Coldwater fish,
such as salmon, are a good source, or you can take 500 mg capsules
twice a day, or simply eat 8-12 ounces of fish per week.
3. Diabetic Low Glycemic Index
Diet:
Dietary control of diabetes comes
down to 2 simple principals:
a. Eat less (less
calories) to maintain ideal body weight.
b. Eat low glycemic index foods that does not turn into sugar
quickly
The Glycemic Index (GI)
The
glycemic index represents the magnitude of the increase in
blood glucose that occurs after ingestion of the food. This
index measures how much your blood sugar increases in the two
or three hours after eating.
When you make use of the glycemic index to prepare healthy meals,
it helps to keep your blood sugar levels under control. GI tends
to be lower for foods that are present in relatively large
particles, minimally processed, and are ingested along with fat
and protein.
Below is the general guidelines to what is high or low Glycemic
Index (GI) foods.
High GI Foods
The following foods are considered unacceptable:
· Foods containing sugar, honey,
molasses, & corn syrup.
· Breads - all white breads, all white flour products, corn breads
· Grains - rice, rice products, millet, corn, corn products
· Cereals - all cereals except those on the Low GI List below
· Pasta - thick, large pasta shapes
· Fruits - bananas, watermelon, pineapple, raisins
· Vegetables - potatoes, corn, carrots, beets, turnips, parsnips
· Snacks - potato chips, corn chips, popcorn, rice cakes, pretzels
· Alcohol - beer, liqueurs, all liquor except red wine
Low GI Foods
Look at what you can have:
· Breads - whole rye, pumpernickel, whole wheat pita
· Grains - barley, bulgur, kasha
· Cereals - Special K, All Bran, Fiber One, regular oatmeal
· Pasta - whole-wheat pasta, bean threads
· All meats
· All dairy products (no sugars)
· Whole Fruits - all except the High GI fruits above
· Green leafy Vegetables - all except the High GI vegetables listed
above
· Snacks - nuts, olives, cheese, pita chips, fried pork rinds
· Alcohol - red wine
· Misc. - olives, eggs, peanut butter (no sugar)
Anti-Aging Food Pyramid for
Diabetes
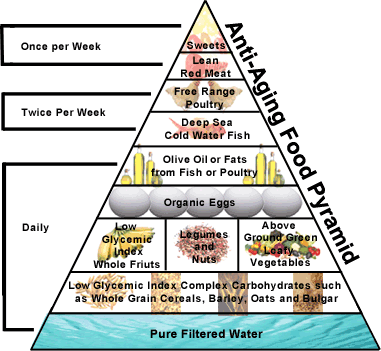
This Diet consists of 50-55% complex
carbohydrates of low glycemic type (whole fruits, above ground
vegetables, whole
grains), 20-25% protein (preferably from plant sources), 25-30%
fat. The normal 5% sweets, candies and dessert should be avoided.
There are three major layers to the Anti-Aging Food Pyramid.
They are divided into daily, 2-3 times a week, and weekly layers.
Imagine a pyramid with three layers, each layer getting much narrower
as it gets closer to the tip.
The daily broad base layers of the pyramid starts
with 10 glasses of pure filtered water a day and complex carbohydrates
supplying up to 55% of the calories These carbohydrates are those
of low glycemic index type - barley, cereal, legumes, and above
ground vegetables. A limited amount of nuts, which is a fatty
food, is also included in this first base layer. Three servings
of vegetables should be taken daily. High glycemic index complex
carbohydrates such as wheat, rice, and corn should be restricted.
Moderate amount is acceptable if they are mixed with fat and
protein.
Egg
forms also part of the base layers. It is a good protein source.
One egg per day is acceptable (including those used in cooking
and baking). Organic eggs are the best.
Olive
oil and fats from fish; nuts are part of this daily layer.
25-30% of the calories in your comes from fats. The fats in the
diet should come mainly from olive oil, which is high in monounsaturated
fats and also a good source of antioxidant. Some comes from the
fish, poultry and meat consumed.
The second layer is a much smaller layer contains
protein food from fish and poultry. You should eat from this group
2-3 times a week. Fish
should be those that live in deep and cold water, such as salmon
and tuna. Poultry
should preferably come from free-range chicken.
The third layer, which is very small, contains foods
that one should eat 1 time a week. These include sweets, red
meat (lean). If blood sugar is severely impaired, sweets should
be avoided altogether.
Diet Tips for Diabetes Mellitus
a. Reduce overall
fat, especially trans-
fat commonly
found in fried food so the overall calories is immediately reduced,
as a result, weight loss is inevitable. Use oils or foods that
are high in Omega-3 fatty acid, such as olive oil, rapeseeds oil,
flaxseed and flaxseed oil, for they lower insulin requirements.
b. Eliminate refined carbohydrates and sugar from
your diet, as they increase the blood sugar immediately. Substitute
complex carbohydrates that have lots of fiber. Beware that sweet
snacking is a frequent behavior at times of stress. Fruit should
be the major source of sweetness in your diet, as they are low
in calories, high in fibers, and many other minerals and vitamins
which are essential for keeping the body healthy.
c. Watch the glycemic Index (a
rating system to measure food's effects on blood sugar levels)
of the carbohydrates that you consume. The higher the glycemic
index, the more pronounced the food will have on your blood sugar,
and scientific studies have shown that leads to excessive food
intake in obese subjects.
d. Celery, Bitter Melon, Onion,
Garlic, Globe Artichoke, Jerusalem artichoke, Asparagus and Spinach
are vegetables that alleviate Diabetes Mellitus.
f. Refrain from excessive protein
in your diet. Try meat substitutes or non-animal protein
foods such as legumes tofu. Eat more fish, chicken and very little
red meats (12-16 oz. per month). Legumes are excellent insulin
regulators.
g. Split your menu into 6 small
meals per day, rather than the traditional 3 square
meals. This way, you will maintain a balance in your blood sugar
and the level of nutrients in your body throughout the day.
4 . Exercise
No diabetes program is complete without a well-balanced
exercise program. While most
people think of exercise as a way to reduce body weight (especially
since 80% of diabetes are obese), exercise
does much more, including reducing
insulin resistance and impotence.
Numerous studies have confirmed that exercise
can cause a reduction in insulin resistance and thus diabetes.
For example, a study was conducted on 5,159 men aged 40 to 59
years with no history of coronary heart disease, type 2 diabetes
or stroke. During an average follow-up period of 16.8 years, there
were 616 cases of major coronary heart disease cases and 196 incident
cases of type 2 diabetes. Risk decreased progressively for type
2 diabetes, according to the Archives of Internal Medicine
2000 (160:2108-2116).
A well-balanced exercise must include three components:
a. Flexibility
training
b. Cardiovascular
training.
c. Strength
training.
Ideally, about 2000
calories should be burned per week. Working out with
30 minutes of aerobics exercise at moderate intensity 5 times
a week plus 15-20 minutes of strength training 3 times a
week will accomplish this goal.
5. Prescription Medications
If the above protocol fails, drugs and insulin have to be used.
Oral Medications commonly prescribed fall into one of 4 categories:
A. Medications that Increase the Insulin Output by the Pancreas,
such as chlorpropamide and tolbutaminde, glyburide, glipizide,
and glimepiride.
B. Medications that decrease the amount of glucose coming from
the liver such as metformin (Glucophage). Metformin
does not alter concentrations of insulin in the blood and, therefore,
rarely causes low blood glucose levels.
C. Medications that increase the sensitivity of cells to insulin,
such as Troglitazone (Rezulin) which was taken off the market
in March 2000 due to liver toxicity, or rosiglitazone (Avandia)
whose long-term safety profile is not known.
D. Medications that Decrease the Absorption of Carbohydrates
from the Intestine such as Precose. Precose has significant gastrointestinal
side effects. Abdominal pain, diarrhea, and gas are common and
are seen in up to 75% of patients.
Summary:
Type 1 Diabetes Mellitus is a disease that requires insulin to sustain
life.
Type 2 Diabetes Mellitus (NIIDM)
is a disease that is largely curable.
Treatment of NIIDM from a drug-free
perspective includes a protocol consisting of 3
steps taken concurrently:
1. Diet of low glycemic index food
to reduce sugar imbalance.
 2. Exercise to maintain ideal body
weight and reduce insulin resistance. 2. Exercise to maintain ideal body
weight and reduce insulin resistance.
3. Nutritional Supplements, including:
Chromium Polynicotinate 400- 1200 mcg a day, Vitamin C 1- 2 grams
a day, Vitamin E 800-1200 I.U. a day, and magnesium 200-300 mg
two to three times a day.
Auxiliary supplements include alpha lipoic acid 300-500
mg a day, bitter melon 2 ounces a day, blueberry 25 mg two times
a day, vitamin B12 500- 2000mcg a day, and gingko biloba 40 to
80 mg three times a day.
If the above fails to control blood sugar, prescription medications
should be considered. Conversely, those who are already on medications
may be weaned off slowly under the supervision of a physician
and following the above protocol.
About The Author
Michael Lam, M.D., M.P.H.,
A.B.A.A.M. is a specialist in Preventive and Anti-Aging Medicine. He is currently
the Director of Medical Education at the Academy of Anti-Aging
Research, U.S.A. He received his Bachelor of Science degree from
Oregon State University, and his Doctor of Medicine degree from
Loma Linda University School of Medicine, California. He also
holds a Masters of Public Health degree and is Board Certification
in Anti-aging Medicine by the American Board of Anti-Aging Medicine.
Dr. Lam pioneered the formulation of the three clinical phases
of aging as well as the concept of diagnosis and treatment of
sub-clinical age related degenerative diseases to deter the aging
process. Dr. Lam has been published extensively in this field.
He is the author of The Five Proven Secrets to Longevity
(available on-line). He also serves as editor of the Journal
of Anti-Aging Research.
For More Information
For the latest anti-aging related health issues,
visit Dr. Lam at http://www.drlam.com/. Feel free to
email Dr. Lam at dr@DrLam.com
if you have any questions.
© 2001 Michael Lam, M.D. All
Rights Reserved.
References:
Modern Nutrition In
Health and Disease, Eighth Ed., 1994. Shils, Olson and Shike,
eds
Abraham AS, et al.: The effects of chromium supplementation on
serum glucose and lipids in patients with and without non-insulin
dependent diabetes. Metabolism 41:768-771, 1992.
Allen, FM: Blueberry Leaf Extract: Physiologic and Clinical Properties
in Relation to Carbohydrate Metabolism. JAMA 89:1577-81, 1927.
Anderson R, et al.: Beneficial effects of chromium for people
with Type II Diabetes. Diabetes. 45(Suppl. 2):124A.
Anderson R: Chromium metabolism and its role in disease prevention
in man. Clin Physiol Biochem. 4(1):31-41, 1986.
Anderson RA, et al.: Supplemental chromium effects on glucose,
insulin, glucagon, and urinary chromium losses in subjects consuming
low-chromium diets. Am J of Clin Nutr. 54:909-916, 1991.
Anderson, R. A., et al. Chromium supplementation of human subjects:
Effects on glucose, insulin, and lipid variables. Metabolism.
32:894-899, 1983.
Anderson, RA, et al. Elevated intake of supplemental chromium
improves glucose and insulin variables in individuals with type
2 diabetes. Diabetes (1997) 46:1786-1791.
Araki, A, et al.: Plasma homocysteine concentrations in Japanese
patients with non-insulin-dependent diabetes mellitus: Effect
of parenteral methylcobalamin treatment. Atherosclerosis. 103:149-157,
1993.
Baskaran, K, et al.: Antidiabetic effects of a leaf extract from
Gymnema Sylvestre in non-insulin-dependent diabetes mellitus patients.
J of Ethnopharmacology. 30:295-305, 1990.
Basualdo, CG, et al. Vitamin A (retinol) status of first nation
adults with non-insulin-dependent diabetes mellitus. J Am Coll
Nutr. 16(1):39-45, 1997.
Bever, B and Zahnd, G: Plants with Oral Hypoglycemic Action. Quart
J Crude Drug Res 17:139-96, 1979.
Bilberry - the vision herb. Mediherb Professional Review. Number
59. August 1997.
Chromium supplements judged safe. Food Chemical News. November
17, 1997, pp 9.
Cohen, N, et al.: Oral vanadyl sulfate improves hepatic and peripheral
insulin sensitivity in patients with non-insulin-dependent diabetes
mellitus. J of Clin Investigations. 95(6):2501-2509, 1995.
Davies S, et al.: Age-related decreases in chromium levels in
51,665 hair, sweat, and serum samples from 40,872 patients - implications
for the prevention of cardiovascular disease and type II diabetes
mellitus. Metabolism. 46(5):469-473, 1997.
Eibi, NL, et al.: Hypomagnesemia in type II diabetes: Effect of
a 3-month replacement therapy. Diabetes Care. 18:188, 1995.
Estrada, EH, et al.: Stimulation of glucose uptake by the natural
coenzyme a-lipoic acid/thioctic acid. Diabetes. 45:1798-1804,
1996.
Evans GW: The effect of chromium picolinate on insulin controlled
parameters in humans. Int J Biosocial Med Research. 11:163-180,
1989.
Friday KE, et al.: The effect of omega-3 fatty acid supplementation
on glucose homeostasis and plasma lipoproteins in type II diabetic
subjects. Am J of Clin Nutr. 45:871, 1987.
Gaby AR, et al.: Nutritional Therapy in Medical Practice: Reference
Manual and Study Guide. Wright/Gaby Seminars, Kent, Washington.
Pages 54-64, 1996.
George Washington University, Department of Pharmacology, Washington,
D.C., Chromium Toxicity Study, 1995
Glauber H, et al.: Adverse effect of omega-3 fatty acids in non-insulin
dependent diabetes mellitus. Ann Intern Med. 108:663-668, 1988.
Henricksson, J, et al.: Influence of exercise on insulin sensitivity.
J Cardio Risk 2(4):303-309, 1995.
Jacobs, S, et al.:Enhancement of glucose disposal in patients
with type 2 diabetes by alpha-lipoic acid. Drug Res. 45:872-874,
1995 .
Kaats, G. R., et al.: Effects of chronium picolinate supplementation
on body composition: A randomized double masked, placebo controlled
study. Curr Ther Res. 57:747-756, 1996.
Krone CA , Ely JT: Vitamin C and glycohemoglobin revisited. Clin
Chem, 47(1): 148 2001
Lee NA, et al.: Beneficial effect of chromium supplementation
on serum triglyceride levels in NIDDM. Diabetes Care. 17:1449-1452,
1994.
Manzella D, Barbieri M, Ragno E, Paolisso G: Chronic administration
of pharmacologic doses of vitamin E improves the cardiac autonomic
nervous system in patients with type 2 diabetes Am J Clin Nutr
73: 1052-1057. 2001
Mertz W, et al.: Present knowledge of the role of chromium. Federation
Proceedings. 33:2275-2280, 1974.
Miller, JC, et al.: Replacing starch with sucrose in a high glycaemic
index breakfast cereal lowers glycaemic and insulin responses.
Eur J Clin Nutr 48(10):749-752, 1994.
Murray, M and Pizzorno, J: Encyclopedia of Natural Medicine. Rocklin,
CA: Prima Publishing, 1998.
Nadler, JL, et al.: Magnesium deficiency produces insulin resistance
and increased thromboxane synthesis. Hypertension 21(6 Pt 2):1024-1029,
1993.
Okabayashi, Y, et al.: Effect of Gymnema sylvestre, R.Br. on glucose
homeostasis in rats. Diabetes Res Clin Pract. 9(2):143-148, 1990.
Paolisso G, et al.: Metabolic benefits deriving from chronic vitamin
C supplementation in aged non-insulin dependent diabetics. J Am
Coll Nutr Aug 14:4 387-92, 1995.
Paolisso, G, et al.: Improved insulin response and action by chronic
magnesium administration in aged NIDDM subjects. Diabetes Care.
12:265-269, 1989.
Schroeder HA: Serum cholesterol and glucose levels in rats fed
refined and less refined sugars and chromium. J Nutr. 97:237--242,
1969.
Sparkman DR: Chromium picolinate safety. All Natural Muscle Development.
35(6):40, 1998.
Tutuncu NB, Bayraktar M, Pehlivanoglu B: The effect of vitamin
E supplementation on erythrocyte osmotic fragility in diabetic
patients. Clin Hemorheol Microcirc 20(3):201-7, 1999.
U. S. Dept. of Agriculture, Human Nutrition Research Center, Chromium
Study, 1996
United States Department of Agriculture. Agricultural Research
Service Quarterly Report of Selected Research Projects. Jul-Sept,
1997.
Wagh, SS, et al.: Mode of action of lipoic acid in diabetes. J
of Bioscience. 11:59-74, 1987.
Welihinda, J, et al.: The insulin-releasing activity of the tropical
plant Momardica charantia. Acta Biologica Medica Germania. 41:1229-1440,
1982.
Welihinda, J, et al.: Effect of Momardica charantia on the glucose
tolerance in maturity onset diabetes. J of Ethnopharmacology 17:277-282,
1986.
Ziegler, D, et al.: Effects of treatment with the antioxidant
alpha-lipoic acid on cardiac autonomic neuropathy in NIDDM patients.
A 4-month randomized controlled multicenter trial (DEKAN Study).
Diabetes Care. 20(3):369-373, 1997.
|
|