|
Cholesterol
Contents:
Cholesterol Basics
Cholesterol and Free Radical Activity
Lipoprotein(a)
Cholesterol and Cardiovascular Disease
What is "Normal" Cholesterol Level?
Cholesterol Lowering Drugs
Diet Cholesterol and Blood Cholesterol
Sugar and Cholesterol
High Cholesterol - a Symptom and NOT a Disease
Cholesterol Lowering Protocol
1. Nutritional Supplements
2. Modified Mediterranean Diet
Diet Tips for Lowering Cholesterol
3. Exercise
4. Natural Lower Cholesterol Agents
Laboratory Standard
Summary
High total serum cholesterol and
LDL cholesterol are significant risk factors of cardiovascular
disease. 14 million American have heart disease and
more than 2,600 die daily from heart attacks in the United States
alone. 15% of adults in their late 30s to 40s are afflicted by
cardiovascular disease, about 50% of 55 to 64- year-oIds, and
65% of those in the next decade.
Developed countries have shown a decrease in dietary fat
and cholesterol consumption in recent years. This is largely
the result of on-going massive public health campaign advocating
a low fat, high carbohydrate diet as ideal to bring down blood
cholesterol level to prevent arthrosclerosis. Despite this effort,
the number of people with elevated blood cholesterol continues to increase.
Obviously there are other causative
factors that have not being addressed. In America alone,
over 40 million prescription was written yearly for cholesterol
lowering medications.
After decades of research, nutritionists are still debated on
the etiology of high cholesterol and the best way to bring it
down. Let us take a closer look.
Cholesterol Basics
Cholesterol is a waxy substance consisting of
fats (lipids) and proteins. It is one of the macro-nutrients
necessary for life. Cholesterol made in the liver and is carried
in the blood on carrier molecules called lipoproteins. The main
lipoproteins categories are very-low-density lipoprotein (VLDL),
low-density lipoprotein (LDL), and high-density-lipoprotein (HDL).
Once bound to the carrier HDL, the cholesterol is known as HDL
cholesterol. HDL in effect transports fat from the cell to the
liver. When the HDL cholesterol level is high, it is more cardio
protective. Therefore, HDL cholesterol is considered "good
" cholesterol. LDL is the carrier of oxidized cholesterol
as LDL cholesterol from the liver to cell. Elevated LDL cholesterol
is directly correlated with increased cardiovascular risk. LDL
cholesterol is therefore called the "bad" cholesterol.
Cholesterol, when unoxidized, is an antioxidant and
free radical scavenger in its naturally occurring state.
In fact, unoxidized cholesterol guards the cell membranes' phospholipids
from free radical damage and protect it against atherosclerosis,
cancer, and other free radical attack. Also, cholesterol is a
predecessor to many steroid hormones and vitamin D. It is produced
at the liver at the rate of 3,000 to 4,000 mg a day.
Cholesterol and
Free Radical Activity
While the exact mechanism of how cholesterol affects
our body is still under intense investigation, it is clear that
the unified theory of free radical damage caused by unhealthy
foods such as processed fat and oxidized cholesterol is the most
likely mechanism. Free Radical damage to our blood vessels
is one of the primary causes of atherosclerosis. The
most important cause of free radical pathology is the excessive
dietary fat consisting of processed poly-unsaturated
fatty acid (PUFA) and trans
fat frequently used in fried foods, margarine, cooking oil,
and oxidized cholesterol from commercially prepared foods.
In the event that dietary fat and oil is retrieved from fresh,
whole, and unprocessed foods, no lipid peroxidation will take
place and the cell membrane will remain healthy in a normal cis-configuration
without any free radical damage.
One theory advanced by the late Nobel laureate Dr. Linus Pauling,
together with his research cohort Dr. Matthias Rath, is that the
total serum cholesterol is really an indicator of the amount of
free radical damage in the body. Our body maintains an optimum
level of total cholesterol level as well as a delicate balance
among its subcomponents. A negative feedback mechanism exists
within the body that decreases the rate of endogenous synthesis
when the dietary intake is exceeds what is needed. The total
circulating cholesterol remains relatively constant at between
170-200 mg/dl for the normal adult. The
higher the free radical level, the higher the body needs to produce
cholesterol internally from the liver to act as an antioxidant
and free radical scavenger. Cholesterol level is therefore
an indicator of free radical activities in the body.
Free radicals are not all bad. Some of it is definitely
necessary to protect us against cancer cells and infections. In
fact, a low total cholesterol level (below 150 mg/dl) has been
linked with an increased risk of cancer and stroke. Too much free
radical, on the other hand, is detrimental to our health.
Cholesterol in its natural state is therefore actually good for us.
During commercialization, lipid (including fat and cholesterol)
peroxidation takes place as soon as fats and oils are extracted
from the foods in which they naturally occur. This commercialization
process is speeded up by metallic ions, particularly iron and
copper. Extensive lipid peroxidation can occur without an apparent
stale or flavor, like in peanut butter, the making of salad and
cooking oil, and also in so-called cold-pressed oils. During the processing of PUFAs to make cooking oil, rapid peroxidation
can take place and free radicals are released. This
process is accelerated by heat, atmospheric oxygen, light, and
trace amounts of unbound metallic elements.
Oxidized cholesterol is a free radical generator. It
is attached particularly to low-density lipoproteins as LDL cholesterol
as it goes from the liver to the cell. Hamburgers and
other cooked and processed foods contain animal fats that are
usually high in oxidized cholesterol when cooked. Foods cooked
in animal fat and fried in processed PUFA (such as corn oil) also
have high oxidized-cholesterol content. As a result, the higher
the LDL cholesterol level, the higher the risk of cardiovascular
disease. Research has shown that rabbits that consumed a small
amount of oxidized cholesterol for merely 12 weeks had atherosclerosis
plaques that were two times as big as the control population.
Studies reveal that heart attack risk falls 2% for every 1% drop
in LDL cholesterol level.
One of the most important causes of free radical pathology is
the excessive dietary
fat consisting of processed PUFA or trans fat frequently used
in fried foods, margarine, and cooking oil. In the event that
dietary fat and oil is retrieved from fresh, whole, and unprocessed
food, no peroxidation will take place and cell membrane will remain
healthy in a normal cis-configuration without any free radical
damage. Studies have shown that 20% of dietary calories as commercially available
fat will not surpass the control threshold of endogenous free
radical protection. Unfortunately, the current contribution from
such commercially processed fat to our diet exceeds 40 percent.
Lipoprotein(a)
Some of the natural cholesterol produced by the liver in response
to free radical damage is converted into LDL cholesterol and its
relative lipoprotein (a) (Lp (a)). While LDL cholesterol maybe
known as the "bad" cholesterol,
Lp (a) is even worse. Lp(a) is a plasma lipoprotein
that structurally resembles LDL, but with an additional adhesive
protein. Lp(a) is also made in the liver and transported to the
cell. Studies have shown that Lp(a) holds fast to damaged blood
vessel, attracting other Lp(a) molecules, and finally constituting
the atherosclerotic plaques. In fact, a high Lp (a) level (more than 30 mg/dl) has been revealed
to carry a 10 times greater risks for heart disease than LDL cholesterol
level. Lp(a) level should be part of a routine blood
screening test for cardiovascular disease risk.
Lp(a), according to Drs. Pauling and Rath, is the body's way of
repairing its damaged vessel wall that has micro leakages caused
at least in part by free radical damage and vitamin deficiencies
(more specifically vitamin C) Humans
do not make any endogenous vitamin C and have no self-repair
mechanism of the vascular system. Lp(a) is used by the body as
a surrogate vitamin C, so to say. Lp(a), unfortunately, has a
sticky characteristic and adheres to each other, forming an atherosclerotic
plaque over time. The body, at the interim, is unaware. As long
as the damage persists due to free radical presence (either from
improper diet, aging, pollution, lack of vitamins, or toxins),
the body responds by making more cholesterol endogenously in the
liver, feeding a viscous cycle of ever increasing Lp(a).
Cholesterol and Cardiovascular
Disease
The notion that total blood cholesterol level alone is the key
determinant of cardiovascular heath should be dispelled. Polar
bears, for example, maintain total blood cholesterol of over 400
mg/dl and they seldom develop heart attacks. There
is obviously a lot more to learn about cholesterol and its link
to cardiovascular disease that we currently know.
It is proven that single focused
dietary strategy of lowering dietary cholesterol does not reduce
coronary heart disease risks. To make matters worse, "low-fat, high carbohydrate" diets are often high in
the wrong type of carbohydrate. Instead of taking in complex,
paleo type carbohydrates such as green leafy vegetables of low
glycemic index, the ignorant consumer often ends up carbohydrates
of high glycemic index such as pasta, soda, processed foods, and
fast foods. These types of food are rich in sugar and starch (carbohydrate).
They actually lower the important "good" HDL cholesterol. A low
HDL cholesterol level is inversely proportional to the cardiovascular
disease risk. It should be remembered that cholesterol and
fat are concentrated sources of calories and can lead to obesity
if consumed too much.
In the Framingham study for example, men and women consumed an
average cholesterol intake of 700 mg and 500 mg per day respectively
were studied (one egg provides 200 mg). The average serum concentration
of cholesterol for men and women with higher than average cholesterol
intake were found to be 237 and 245 mg/dl respectively. Subjects
with lower than average intakes were found to be 237 and 241 mg/dl.
The difference is statistically insignificant. Statistically,
studies have showed that people who consume 4 eggs per week (one egg provides 200mg cholesterol)
actually have average serum cholesterol (193 mg/dl) same than
those who reported consuming only 1 egg per week (197 mg/dl).
Clearly dietary cholesterol in and of itself is not the critical
link to heart disease risks as we once thought.
What is "Normal"
Cholesterol Level?
A low total serum cholesterol level (under 150 mg/dl) is undesirable
for the healthy person. It is very difficult to lower cholesterol
only without other types of fats because they are often found
intermingled with each other in food. While saturated fatty acid
(SFA) from animal and diary products is not subject to lipid peroxidation,
all animal fats contain some PUFA and cholesterol, both of which
undergo auto-oxidation. Those who are serious in reducing total
serum cholesterol level should refrain from intake of lipid peroxide-containing
fats (trans fat such as margarine) with resulting reduction of
free radical pathology. Like trans fat, oxidized cholesterol should
be limited as much as possible.
A low fat diet may actually bring harm to health. The
correct way is to discern the right type of fat and cholesterol
to take and those to avoid. The overall fat intake as a percentage of dietary
calories should not fall below 25-30%. One should have plenty of "good" mono-unsaturated
fatty acids (MUFA) like olive oil, seeds, nuts, and cold-water
fish that have high omega-3
fatty acid (N3) content.
Saturated
fat is necessary for good health. It should come from free-range
poultry or beef, and organic eggs. It is very important to avoid
"bad" trans fat, like margarine and fried foods. Moreover, the
use of processed PUFA such as corn, safflower or sunflower oil
should be restricted.
The optimum level of blood cholesterol
should be at the upper end of normal around 200 mg/dl.
Cholesterol Lowering Drugs
A class of drugs used to aggressively treat elevated LDL levels
is the synthetically derived HMG-CoA reductase inhibitors such
as Iovastatin, pravastatin, and simvastatin. They are collectively
called "statin" drugs.
By inhibiting the production of HMG-CoA reductase, cholesterol
production in the liver is reduced. These are among the most potent
lipid-lowering agents available. To compensate for the resulting
reduction of cholesterol production, the liver increases absorption
of LDL cholesterol, further contributing to an overall reduction
of LDL cholesterol levels.
While statin drugs are effective
in lowering LDL cholesterol, they have serious side effects. For
years, the public is led to believe the wonders of statin drugs
not only in lowering cholesterol but posses other health benefits
as well. Millions of statin prescriptions are written yearly in
the United States alone. In August
2001, however, German Pharmaceutical giant Bayer AG withdrew the
cholesterol-lowering statin drug Baycol from the market because
it was linked to 31 deaths. Moreover, deaths occurred at the manufacturer's
recommended initial dose (0.4 mg/day) as well as at the highest
dose (0.8 mg/day). The majority of deaths occurred
in elderly patients and more often in women.
There are other statin drugs on the market, such as Lipitor (the
best seller). Like Baycol, these drugs are linked to the same
rare muscle weakness, known as myositis, which occurs in about
1 in 1,000 statin users. Myositis occasionally progresses to rhabdomyolysis
-- a complete breakdown of muscle cells that can lead to kidney
failure and death. Some experts believe that pravastatin (Pravachol)
and fluvastatin (Lescol) may have less potential for this deadly
drug interactions. The data at this time are not sufficient to
declare one statin drug safer or more dangerous than the others.
Statin drugs also inhibits the intrinsic
biosynthesis of Coenzyme Q10 (CoQ10), a central compound
in the mitochondrial respiratory chain. CoQ10 is indispensable
for optimum cardiac function. Reduction of CoQ10 constitutes new
risk of cardiac disease, especially for those whose cardiac function
is compromised, such as those with congestive heart failure or
cardiomyopathy.
Furthermore, statin drugs have been linked to various forms
of cancer in laboratory animals. It will be years before we
know the full side effects of statin drugs.
Using statin drugs on a short-term basis to normalize
blood cholesterol is a reasonable alternative if a drug-free approach
fails. Anyone on long term statin type cholesterol lowering drug
would be wise to get regular checkups, especially on liver function.
Diet Cholesterol and Blood
Cholesterol
The trend to reduce serum total and LDL cholesterol started in
the past two decades when studies linked high dietary saturated
fat intake to increased serum cholesterol level. Furthermore,
studies have convincing shown that a high LDL cholesterol level
is a definite risk factor and increases chances of cardiovascular
disease. Furthermore, cholesterol lowering statin drugs such as
Lipitor is effective to reduce LDL cholesterol. The solution therefore
appears simple - reduce dietary cholesterol on the presumption
that high dietary cholesterol leads to high LDL cholesterol. If
that fails, prescribe cholesterol-lowering medication.
The reality is that studies have
shown that a diet high in cholesterol will
not lead to high blood cholesterol if the subject is healthy.
Blood cholesterol level only increases by 3 mg/dl after ingestion
of one egg day for a continuous period of 6 weeks (one egg contains
about 230 mg of cholesterol) in repeated studies. Clearly,
dietary cholesterol is not the main
culprit.
Sugar and Cholesterol
Sugar consumption has been increasing for the past 100 years and
this upward trend remains unabated. Increase rate of cardiovascular disease has a directly
correlation to the increase in sugar intake and not fat and cholesterol
intake. Sugar
includes grains such as wheat and rice. Also included are
starchy underground vegetables such as potato, yam and carrot
that convert quickly into sugar once inside the body.
High sugar intake is linked to an increased risk of heart disease.
Simple sugars are the primary source
of high triglycerides, a type of blood fat, and very low-density
lipoproteins (LDL), which are an independent risk factor for atherosclerosis.
Sugar lowers good HDL cholesterol and raises bad LDL
cholesterol and blood pressure levels. It is estimated that
a high sugar intake may account for as many as 150,000 premature
deaths from heart disease in the US each year.
Sugar increases triglyceride storage
and cellular oxidative damage. This assaults the vascular
wall, leading to micro-leakages in the endothelial wall of blood
vessels, leading to the self-repair mechanism of cholesterol and
lipoprotein (a) production described above. Sugar is therefore
a significant contributory factor of oxidative stress. Simple
logic dictates that reduction of
sugar intake will reduce oxidative stress. This in turn will reduce
cholesterol production from the liver.
Studies have been conducted to support this. In one research trial,
18 male subjects received normal food followed by a rigorously
specified diet in which protein and carbohydrate requirements
were met by amino acids, essential fat, and glucose. The average
concentration of cholesterol in the initial period, on normal
food, was 227 mg/dl. After two weeks on the restricted glucose
diet, it had dropped to 173. Two weeks later, the level was at
160. When the diet was altered by replacing 25 percent of the
glucose with sucrose (while all other dietary constituents kept
constant), the average cholesterol level rose from 160 to 178
within one week and to 208 within two weeks. The researchers carried
the study one step further. The sucrose was replaced with glucose
again. With this change, the cholesterol concentration dropped
back to 175 within one week and the decline continued. It finally
leveled off at 150 mg/dl, which was 77 mg/dl less than the initial
value. This research finding links the consumption of sucrose
(table sugar) directly to increased cholesterol. The exact
mechanism is still under research.
In addition to glucose, fructose from fruits also raises blood triglyceride level.
In a clinical trial conducted at the University of Minnesota,
researchers followed 24 healthy adults who received one of 2 diets
assigned randomly for a period of 6 weeks and then switched back
to the other diet for 6 weeks. One diet provided 17% of energy
as fructose and the other diet was sweetened with glucose and
was absent of fructose. Both diets contain common foods and contained
nearly identical amounts of the macronutrients. The researchers
found that in men, the fructose diet raised plasma triglyceride
levels by 32%, although there was no effect seen with the
women being studied.
Elevated triglyceride blood level of in itself is a strong and
independent risk factor for heart attack among middle-aged and
elderly men. In fact, studies have shown that blood triglyceride
level was a stronger risk factor than total cholesterol alone.
It is not known why women appear to be immune to this other than
postulations that the high level of estrogen acts as a protective
factor. The exact mechanism is still under investigation.
High Cholesterol -
a Symptom and NOT a Disease
Elevated cholesterol is a symptom and not a disease. The real problem is oxidative damage from
excessive free radical damage caused by excessive metabolism of
oxygen and sugar. Human lacks the endogenous capacity to produce
vitamin C, a natural anti-oxidant. Instead, the body produces
cholesterol as a surrogate. If you understand this concept, it
is easy to appreciate that high cholesterol and a host of other
age- related diseases such as arthrosclerosis
is nothing more than a series of symptoms reflective of the body's
response to imbalanced oxygen and sugar metabolism. To normalize cholesterol level permanently, proper
control of your oxygen load (through reduction of oxidative stress
by taking anti-oxidants) and sugar load (by
avoiding foods that are high in sugar and concentrate on low glycemic
index food) is the first and most important step, in addition
to exercise. related diseases such as arthrosclerosis
is nothing more than a series of symptoms reflective of the body's
response to imbalanced oxygen and sugar metabolism. To normalize cholesterol level permanently, proper
control of your oxygen load (through reduction of oxidative stress
by taking anti-oxidants) and sugar load (by
avoiding foods that are high in sugar and concentrate on low glycemic
index food) is the first and most important step, in addition
to exercise.
Cholesterol Lowering Protocol
Unless you have high cholesterol due to familial
factors, lowering plasma LDL cholesterol can be achieved effectively
by eliminating the two key causative factors - excessive oxidation
and sugar overload. This is best done through a combination of
nutritional supplementation, diet, and lifestyle modifications.
Steps
1,2, and 3, when taken concurrently,
will lower your cholesterol within
30 to 60 days. These three steps
can be continued on an on-going basis.
Step
4 contains specific natural
cholesterol lowering agents that can be used for short term to
reduce cholesterol level if you wish more
potent action. It can added after steps 1,2, and
3 fails. This is not a mandatory step but an option. Long
term use of this step should be supervised by a knowledgeable
health professional.
1. Nutritional Supplements
A. Coenzyme Q10 (CoQ10)
is a foundation formula to that enhances mitochondrial function.
CoQ10 supports
healthy HDL and prevents the excess oxidation of LDL. Statin drugs
reduce the level of CoQ10 in the body. Dosage: 30-90 mg daily.
B. L-carnitine, which
works synergistically with CoQ10 to support healthy cholesterol
and improves transportation of nutrients from the extra-cellular
space to the intra-cellular space. Dosage: 250 -1,000 mg daily.
C. Garlic reduces triglycerides
and LDL cholesterol. In addition to using fresh garlic in your
cooking (best to let it a fresh garlic sit for 20 minutes in open
air before eating), you can also take a therapeutic dose of garlic
in supplement form. Dosage: varies, depending on the product.
Look for garlic supplements standardized to 12,000-ppm allicin
potential, and aim for at least 6,000 mcg of allicin per day.
This is equivalent to about 4 cloves a day. Garlic has blood-thinning
effect, and should not be taken in high amounts if you are on
blood thinners.
D. Digestive Enzymes
including lipase and amylase helps to breakdown food and aid in
digestion. Bowl transit time is also reduced, with resulting less
stasis and absorption of fat.
E. Probiotics or
"friendly bacteria" such as
L. Acidophilus help promote healthy cholesterol by converting
it into a less absorbable form and sending it down the gastro-intestinal
tract for emptying. It also increase enzyme production such as
proteases that digest proteins and lipases that digest fats. Dosage:
1- 2 capsules a day, between meals.
F. Milk Thistle (Silybum
marianum) known as silymarin, is a group of
flavonoid compounds. Silymarin prevents damage to the liver
by acting as an antioxidant. It is much more effective than vitamin
E and vitamin C. Liver is the major detoxification center
of the body, and silymarin protects this organ against these toxins.
Silymarin also works by preventing the depletion of glutathione.
The higher the glutathione content, the greater the liver's capacity
to detoxify harmful chemicals. In human studies, silymarin
has been shown to exhibit positive effects in treating liver diseases
of various kinds including cirrhosis, chronic hepatitis, fatty
infiltration of the liver, and inflammation of the bile duct.
Dosage: 70 to 200 mg one to three times a day.
G. Herb Tea. Enhanced intestinal motility
is a key factor to optimum digestive health. Herbal ingredients
and commonly used ingredients that enhance intestinal motility
include: senna leaf, peppermint leaf, stevia leaf, buckthorn bark,
damiana leaf, RED peel, chamomile flower, and uva ursi leaf.
It is always good to eat your regular meal fortified with
digestive enzymes to enhance breakdown of food in the gastro intestinal
tract as a routine practice. After the evening meal, you can begin
drinking tea. Start slowly. You should begin by steeping the
tea just 2 minutes (in 1-2 cups of water) for the first 3-5 days.
As your system adjusts, you may increase steeping to 5 minutes.
Most individuals will experience increased bowel movements or
slight cramping during the first few days. This is due to the
initial cleansing of the body system and is normal.
2. Modified Mediterranean Diet
The
surest way to reduce cholesterol is by reducing
sugar intake and not reducing
dietary cholesterol alone.
While we cannot live with sugar, excessive sugar intake leads
to increased oxidative stress, triglyceride formation and rising
cortisol level. In addition to causing the rising of cholesterol
production from the liver, these are all pro-aging factors as
well.
The anti-aging pyramid is a simple graphic format based on the
modified Mediterranean Diet. It will reduce blood cholesterol
level by reducing unnecessary sugar intake while supplying optimum
nutrition. This food choice program consists of 50-55% complex
carbohydrates of
low glycemic index type food such as legumes, nuts, whole-wheat,
and whole fruits, 20-25% protein (preferably from plant sources),
25-30% fat, and 5% sweets, candies and dessert. This is in
sharp contrast to the typical American diet where 46% comes from
simple
carbohydrate such as white bread and pasta, and 43% of calories
comes from fat (most saturated and trans-fat)
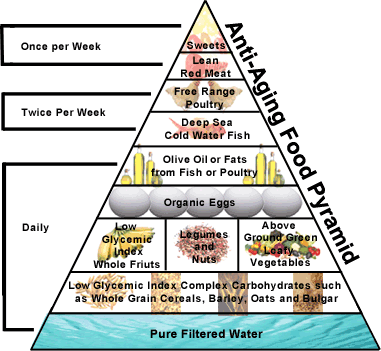
There
are three major layers to the Anti-Aging Food Pyramid.
They are divided into daily intake layers, 2-3 times a week layers,
and once a week layers. Imagine a pyramid with three groups of
layers, each layer getting much narrower as it gets closer to
the tip.
The broad base layers of the pyramid starts with 10 glasses
of pure filtered water a day and complex carbohydrates supplying
up to 55% of the calories These carbohydrates are those of low
glycemic index type - barley, cereal, legumes, and above ground
green leafy vegetables.
A limited amount of nuts, which
is a fatty food, is also included in this first base layer.
Three servings of vegetables should be taken daily. High glycemic
index complex carbohydrates such as wheat, rice, and corn should
be restricted. Moderate amount is acceptable if they are mixed
with fat and protein.
Egg
forms also part of the base layers. It is a good protein source.
One egg per day is acceptable (including those used in cooking
and baking). Organic eggs are the best.
Olive oil and fats from fish; nuts are part of this daily layer.
25-30% of the calories in your comes from fats. The fats in the
diet should come mainly from olive oil, which is high in monounsaturated
fats and also a good source of antioxidant. Some comes from the
fish, poultry and meat consumed.
The second group of layers is a much smaller
layer contains protein food from fish and poultry. You should
eat from this group 2-3 times a week. Fish should be those that
live in deep and cold water, such as salmon and tuna. Poultry
should preferably come from free-range chicken.
The third group of layers ,
which is very small, contains foods that one should eat 1 time
a week. These include sweets, red meat (lean).
Diet Tips for Lowering Cholesterol
a.
Reduce overall fat, especially trans-fat commonly found
in fried foods and margarine. Use oil or food that are high in
Omega-3 fatty acid, such as olive, rapseed oil, flaxseed and flaxseed
oil. Omega-3 fatty acid increase serum HDL Cholesterol. Avoid
polyunsaturated and saturated oil, as they increase the cholesterol
and triglycerides levels. Stay with mono-unsaturated fat such
as olive oil for all cooking needs.
b. Eliminate refined carbohydrates
and sugar from your diet and substitute complex carbohydrates
that have lots of fiber. Fruit should be the major source of sweetness
in your diet. Fruits are filled with pectin and fiber, which work
wonders in lower serum cholesterol.
c. Foods that have been shown to lower LDL cholesterol
include oat bran, oatmeal, and dry beans out of a can.
Oat bran has been shown to reduce LDL cholesterol by up to 20%.
Grapefruit - segments and membranes, not the juice - drives down
cholesterol. Also fresh oranges, apples, garlic, onions,
barley, ginger, and shitake mushrooms.
d.
Eat lots of raw onion - at least half a medium onion a day. This
has been shown to raise the good HDL cholesterol by up to 30%.
Oat bran has also been shown to increase HDL cholesterol by up
to 20%.
If you want a step by step dietary approach, My Detox
Diet Protocol will help you to lower your cholesterol gradually.
You can also pick up many tips on
how to change to a healthier lifestyle by reading my over
100 Anti-aging Strategies.
3. Exercise
No diabetes program is complete with a well-balanced
exercise program. While most
people think of exercise as a way to reduce body weight , exercise
does much more, including reducing
insulin resistance and impotence.
A well-balanced exercise must include three components:
a. Flexibility
training
b. Cardiovascular
training.
c. Strength
training.
Ideally, about 2000
calories should be burned per week. Working out with
30 minutes of aerobics exercise at moderate intensity 5 times
a week plus 15-20 minutes of strength training 3 times a
week will accomplish this goal.
4. Natural Lower Cholesterol
Agents
A.
Soluble Fiber. Psyllium (Metamucil), a natural, water-soluble,
gel-reducing fiber, which is extracted from the husks of blond
psyllium seeds (plantago ovata), is a member of a class of soluble
fibers referred to as mucilage.
Psyllium's total dietary content - 86 percent - is made up of
71 percent soluble fiber and 15 percent insoluble fiber. This
compares to 15 percent total fiber and only five percent soluble
fiber for oat bran. The soluble fiber in one tablespoon of psyllium
is equal to 14 tablespoons of oat bran, another soluble fiber.
For this reason, in contrast to oats, psyllium is added in relatively
small quantities to other cereal grains to make food products.
Numerous studies have found that patients with mild to moderately
elevated cholesterol levels can achieve a sustained reduction
of about 10% in cholesterol level by consuming psyllium twice
a day and adhering to the American Heart Association's
(AHA) Diet.
Numerous landmark studies have been conducted to validate this.
One is cited in the December 1, 1996 issue of the publication
OBGYN News. This study was led by Dr. James Anderson, professor
of medicine at the University of Kentucky College of Medicine
in Lexington. For six months, Dr. Anderson followed 248 patients
who were all instructed to follow the AHA diet. Some patients
were given Psyllium while others were given a placebo. The average
cholesterol level for the study population was 229 mg/dl, with
an LDL cholesterol of 154 mg/dl. After six months, members of
the Psyllium plus diet group lowered their total cholesterol
by 8.6% and their LDL cholesterol by 11.1%, versus those
in the diet group who showed only a 4% reduction in both these
levels. The researchers further note that the Psyllium worked
best for those people with the highest cholesterol levels, with
reductions of up to 25%.
Another well-designed, controlled study followed more than 100
adults with high blood cholesterol (levels greater than 220 mg/dl).
The study followed men and women who ate a high-fat diet (40 percent
or more of total calories) as compare to those who ate a low-fat
diet (no more than 25 percent of total calories). Researchers
then compared the effects of adding 1 1/2 packets of Psyllium
(Metamucil) twice a day on blood cholesterol levels with the effects
of not taking the soluble fiber supplement.
After eight weeks, supplementation with Psyllium showed a small
but significant decrease in total cholesterol and LDL cholesterol
levels, regardless of the type of diet. Total cholesterol levels
dropped a weighted average of 4.7 percent; LDL cholesterol levels
showed a 6.6 percent decrease.
Soluble fiber
causes loose bowl movement and may reduce gastro-intestinal motility
on chronic use. Long term use should be directed under
the supervision of a physician. Dosage: 2 times a day.
B.
Niacin is very effective normalizing cholesterol and
Lp(a), the relative of LDL cholesterol and another independent
and proven risk factor for heart disease. Since therapeutic levels
of niacin is high and can cause an unpleasant
flushing sensation and headache, gradually increase
your dosage over several weeks or use the flush-free form of niacin,
inositol hexaniacinate. Dosage: 100 mg twice daily, increasing
to 500 mg daily. More may be needed under the supervision of a
physician.
 C. Fish oil lowers blood triglyceride levels, may elevate
HDL, and helps support heart health. Most research studies are
based on a high dosage of 3,000 mg. daily. At this
dose, most people developed a harmless fishy
burp after consumption of fish oil pills. If
you take at least 12 ounces of fish a week, fish oils are not
needed. Dosage: 2,000- 3,000 mg C. Fish oil lowers blood triglyceride levels, may elevate
HDL, and helps support heart health. Most research studies are
based on a high dosage of 3,000 mg. daily. At this
dose, most people developed a harmless fishy
burp after consumption of fish oil pills. If
you take at least 12 ounces of fish a week, fish oils are not
needed. Dosage: 2,000- 3,000 mg
Laboratory Standard
From a laboratory test perspective of controlling cholesterol,
the following parameters should be considered optimum:
· Maintain a healthy total cholesterol
level at the upper limit of normal at around 200 mg/dl.
· High HDL level (more than 50 mg/dl) and a low LDL level (less
than 130 mg/dl).
· Total cholesterol /HDL cholesterol ratio of less then 4.
· LDL/HDL cholesterol ratio of less then 2.5.
· Triglyceride level of under 150 mg/dl.
The best way to accomplish is to limit the amount of simple
refined carbohydrates (sugar), processed polyunsaturated fats
(corn oil), and trans fats (donuts and fast foods), while maintaining
a balanced diet of complex carbohydrates of low glycemic index
type (green leafy vegetables that are grown above the ground),
saturated fat from free-range animals (as in meat and butter),
and moderate amount of cholesterol (in meat and eggs)
Summary:
Elevated blood cholesterol is a symptom of rising oxidative stress
and sugar overload. Normalization of cholesterol level to the
upper end of normal range around 200 mg/dl should be the goal.
Too low (below 150 mg/dl) a cholesterol level is undesirable.
A three pronged concurrent approach
is best, consisting of specific nutritional supplementation
, a modified Mediterranean diet focused on low glycemic
index foods, and a well-rounded anti-aging exercise program. Additional
natural agents such as niacin, fiber, and fish oil in high dose
can be added as an adjunct for short term use.
About The Author
Michael Lam, M.D., M.P.H.,
A.B.A.A.M. is a specialist in Preventive and Anti-Aging Medicine. He is currently
the Director of Medical Education at the Academy of Anti-Aging
Research, U.S.A. He received his Bachelor of Science degree from
Oregon State University, and his Doctor of Medicine degree from
Loma Linda University School of Medicine, California. He also
holds a Masters of Public Health degree and is Board Certification
in Anti-aging Medicine by the American Board of Anti-Aging Medicine.
Dr. Lam pioneered the formulation of the three clinical phases
of aging as well as the concept of diagnosis and treatment of
sub-clinical age related degenerative diseases to deter the aging
process. Dr. Lam has been published extensively in this field.
He is the author of The Five Proven Secrets to Longevity
(available on-line). He also serves as editor of the Journal
of Anti-Aging Research.
For More Information
For the latest anti-aging related health issues,
visit Dr. Lam at http://www.drlam.com/. Feel free to
email Dr. Lam at dr@DrLam.com
if you have any questions.
© 2001 Michael Lam, M.D. All
Rights Reserved.
|
|